By Fran Melmed
Employees and employers are set to see double-digit increases again this year.
I’m not sure that’s a shocker anymore. It’s certainly not new. Health care costs have been rising for almost as long as I’ve been writing about them. There are, however, new troubling statistics:
- In 2010, the average family premium ($13,770) is 114 percent higher than it was in 2000.
- Families are paying, on average, 30 percent of the premium, up from 27 percent in 2009 — a greater-than-normal increase in a single year. (Employers’ fell by 0.9%.)
- Earnings have risen only 18 percent. Inflation was 12 percent.

Pile on larger deductibles, more out-of-pocket costs and additional cost-sharing for prescriptions and employees are being squeezed from all sides and are forced to make short-term decisions with long-term ramifications.
Meanwhile, back at the ranch
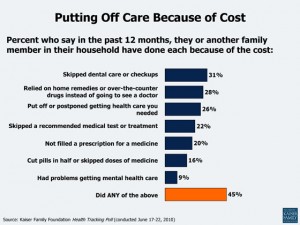 Employees aren’t the only ones wrestling with a bigger cost burden. Employers, too, are feeling the pain. In response:
Employees aren’t the only ones wrestling with a bigger cost burden. Employers, too, are feeling the pain. In response:
• 30 percent of employers reduced their benefits.
• 23 percent increased the share of the premium an employee must pay.
• 74 percent offer at least one wellness program (the increase is primarily driven by smaller firms and attributed to the availability of Web-based resources).
Not surprisingly, companies are ceaselessly tweaking their benefits design to maintain coverage and bend the cost curve.
Every decision directs another
These tweaks, in part, direct what employees do. Or don’t do, as the health care rationing testifies. How companies approach cost pressures and where and how they adjust their strategy will affect employees’ health for years to come.
Are they considering what behaviors their cost or design changes will drive and whether these changes support or clash with corporate messages about health, well-being and mutual responsibility? Are they considering whether the changes will:
- Price out-of-paycheck and out-of-pocket expenses to help keep not only preventive, but routine care within the reach of all?
- Reduce the lack of adherence by making medications and tools free for prevalent chronic conditions?
- Increase health literacy to improve health-related decisions?
- Deliver information and tools that can be understood and used anytime, anywhere?
- Include partnerships, tactics and incentives to remove the easier barriers — time and money — to staying well?
- Examine the attitudes and environmental barriers that get in the way of good health?
Before they shift here, cut there or invest anywhere, companies would be well advised to consider what story they want the results of their health and wellness strategy to tell.
P.S. — If you’re interested in learning more on the topic, the issue of rising health care costs has been covered here at TLNT, and by many others, in great detail.
TLNT contributor Fran Melmed frequently writes about wellness and health care on her Free-Range Communication blog.
